Addressing Unconscious Bias Can Save Lives of Black and Hispanic Infants and their Moms

By Meg Distler, Executive Director, St. Joseph Community Health Foundation
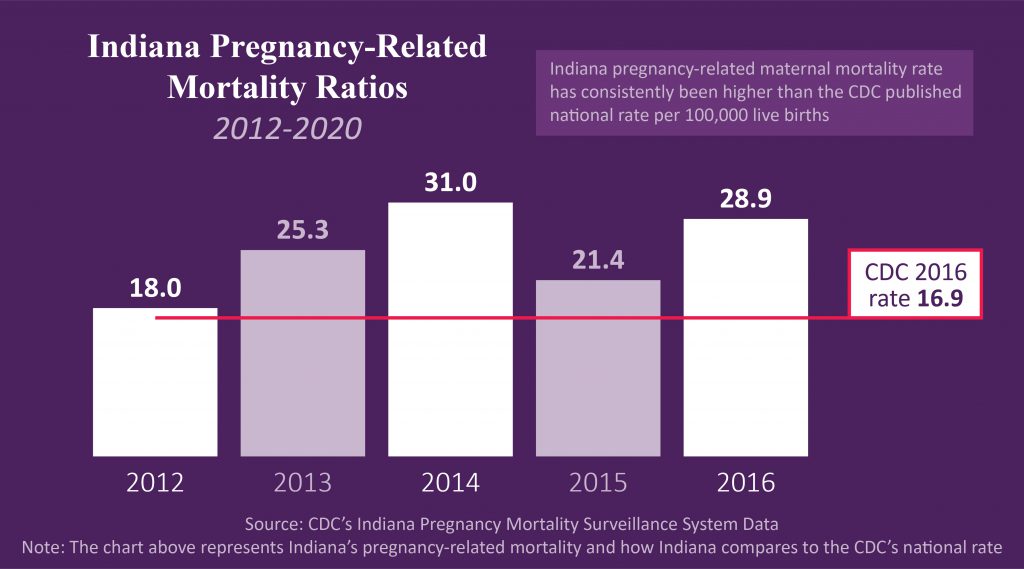
In 2018, Black infants in northeast Indiana were 2.2 times more likely to die before their first birthday. Black mothers had the highest rate of pregnancy-related mortality at 37.0 deaths per 100,000 live births in Indiana for 2012-2016, compared to the national rate of 16.9, according to the Indiana State Department of Health (ISDH). Dr. Nancy Swigonski, MD, MPH, MBA, FAAP (I.U. School of Medicine), commented at a Prenatal & Infant Care Luncheon sponsored by our Foundation in February that Indiana is in crisis. “By the time you wake up tomorrow morning, on average, another baby in Indiana has died. In Allen County, 38 babies died in 2017, which is one baby every nine days, or three babies per month.”
If you look at birth outcomes by race, the crisis is more evident.
These significant disparities in life expectancy and other health outcomes persist across Indiana, the United States, and in our community. Research compiled by the State of Babies Yearbook: 2020 (StateofBabies.org) confirms there are evident racial/ethnic disparities on many indicators among infants, toddlers, and their mothers across the country to varying degrees. The following are facts on Indiana:
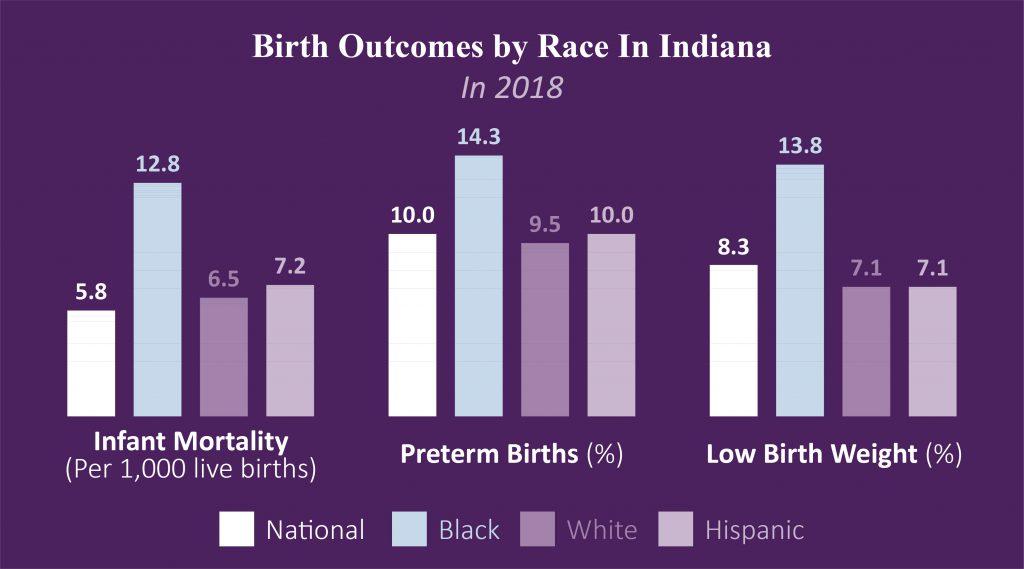
- Infant Mortality: The mortality rate for Black infants (12.8 per thousand births) was about twice the rate for White infants (6.5). Mortality was slightly higher for Hispanic infants (7.2) in Indiana in 2018.
- Preterm Births: The preterm birth rate for Black women (14.3%) in Indiana in 2018 was 51% higher than the rate for White women (9.5%), and the rate for Hispanic women (10.0%) was 5% higher than the rate for White woman.
- Low Birthweight: In Indiana, in 2018, the rate of Black women at risk for having low-weight births (13.8%) was more than twice that for White women (7.1%) and the rate for Hispanic women (7.1%). In 17 states, the birthweight rate for Black women is more than double that for White women.
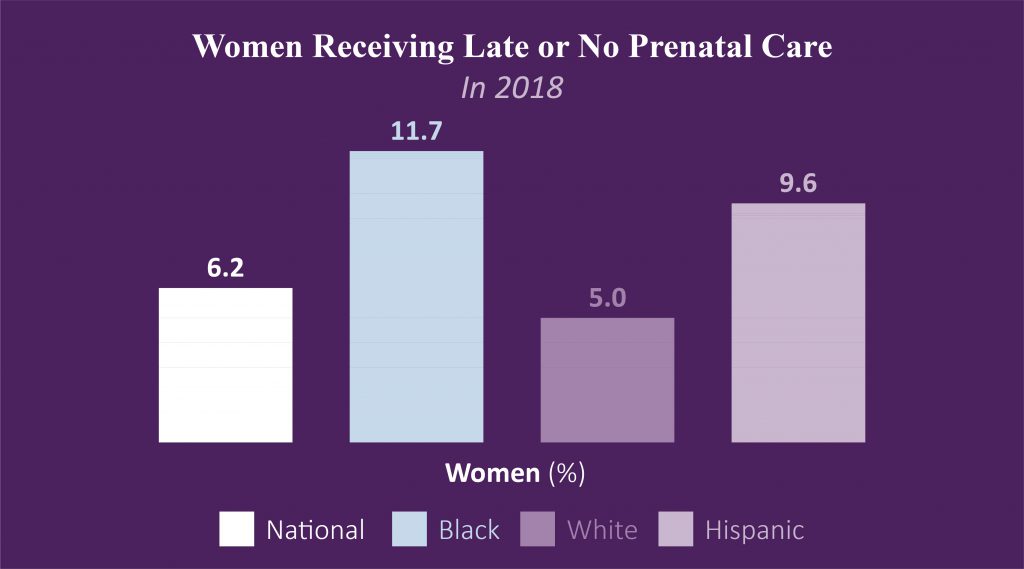
- Prenatal Care: In 2018, while only 5.0% of Hoosier White women received late/no prenatal care, more than twice that number, 9.6% of Hispanic women and 11.7% of Black women received late or no prenatal care.
- Maternal Morbidity and Mortality: Nationally, maternal mortality among Black women (40.8 per 100,000 live births) is more than three times higher than among White women (13.2 per 100,000 live births). Hispanic women had a lower rate (11.6 per 100,000).
What are the causes of racial and ethnic inequities and disparities? Research is abundant, documenting the impact of stressful experiences, racism, and discriminatory practices upon the health of Black and Hispanic women and their families. In addition to stress and racism, women of color disproportionately experience many risks associated with poverty. There is also differential access to medical care and family support services for many women of color. Even when mothers-to-be can access health care, Black or Hispanic women do not always receive equitable treatment from providers.
In a national poll, nearly one-third of Black Americans reported they had personally experienced racial discrimination during a visit with a health care provider.
Stateofbabies.org
Several policies available to states are helping to decrease race-linked differences in maternal health and birth outcomes. Most of these focus on ensuring equitable access to health care, including nutrition, and extending the supports to expectant and new parents. Policies that are influential in addressing the equity gap include those in Medicaid and WIC, among others.
Indiana is making some progress with these policies. For example, Indiana’s Medicaid expansion helped many achieve access, and as of 2018, the Indiana State Department of Health reported that 39.2% of Hoosier moms who gave birth were on Medicaid. Furthermore, only 8.1% of Indiana’s low-income infants/toddlers lack health insurance. While the overall rate has declined, rates are twice as high among Hispanic children. Indiana’s Medicaid policy also recommends maternal depression screenings during well-child visits. This is important to nearly 30% of adults on Medicaid who reported having either a mental disorder or a substance abuse disorder.
Special supplemental nutrition programs for Women, Infants, and Children (WIC) provide valuable support to low-income families. The American Journal for Public Health reported that Black women who were WIC participants experienced markedly lower infant mortality rates. 85.6% of the eligible infants in Indiana participated in WIC in 2016.
What can be done to address health inequities in the health care system? The State of Babies Report recommendations include: Expand training for the health care workforce on the experience of racism in medical care, implicit bias (unconscious attitudes that can lead to negative behavior toward Black and Hispanic people), and culturally competent care.
What is happening here? In 2015, the St. Joseph Community Health Foundation, which is an independent foundation sponsored by the Poor Handmaids of Jesus Christ, began convening Allen County’s prenatal and infant care providers into the Prenatal and Infant Care (PIC) Network. The Network meets quarterly, focusing on increasing awareness amongst care providers of local expertise and resources available for pregnant women and infants. Today, this is a group of over 300 individuals from 90 organizations committed to caring for the over 5,200 babies born in Allen County annually. For the past two years, the group has continually identified the need for more training to address racism, health equity, and health disparities. Responding to these requests, the St. Joseph Community Health Foundation will sponsor two training events facilitated by Aaron and Janel Lane, Cofounders of Courageous Living, Fort Wayne, IN on Race & Cultural Learning for Care Providers on September 2 and 15. The Lanes will explore cultural patterns that create challenges, and how to best address critical conversations and difficult experiences regarding implicit bias on race.
The St. Joe Foundation is also offering scholarship seats for the newly developed March of Dimes, Breaking Through Bias in Maternity Care, on-line, self-paced learning modules. The 75-minute training will be provided to PIC members starting in September. All training events offer data, facts, and insight into the unconscious biases that are occurring in health care today.
Participants in either training are also invited to participate in a follow up facilitated group that will meet after the training events to assist individuals in identifying key strengths and weaknesses with the organization and best practices to address them.
For more information on these training opportunities and other resources for prenatal and infant care providers, visit the St. Joe Foundation website at https://sjchf.org/programs/pic-network/ .
Recent Stories
- $170,600 grant supports resilience and accessibility in the local food system
- The Carriage House: Embracing human dignity through community
- Addressing maternal housing instability, a critical conversation
- Meg Distler Receives 2024 Saint Katharina Kasper Award
- Matthew 25 and St. Vincent de Paul Society partnership makes care more accessible
